A century of progress against cardiovascular disease

When it comes to our health, people typically have a general understanding of what's best.
For instance, we know diet and exercise are important. Sleep, too. And not smoking. And while we may not always remember the ideal numbers for weight, cholesterol, blood pressure and blood sugar, we know they matter.
We know we should get a checkup every year. We also know bad things can happen anyway, especially if they run in the family. And as scary as it is to imagine having a heart attack, we probably also know at least one survivor. Odds are we even know someone who survived without needing open-heart surgery; they likely got a stent or two. They might've even gone home from the hospital the next day.
Hopefully we know how to B.E. F.A.S.T. to spot the signs of a stroke. That is, if we detect someone with (b)alance loss, (e)ye (vision) changes, (f)ace drooping, (a)rm weakness or (s)lurred speech, it's (t)ime to call 911.
We're familiar with CPR and perhaps even learned how to do it, maybe as a requirement to graduate high school or for a job. Learning CPR probably also meant learning about AEDs, those small boxes that can shock a heart back into action.
While we could keep spooling this forward, let's go the other direction.
Think back 10 … 25 … 50 … 75 … 100 years ago. To "a time of almost unbelievable ignorance about heart disease," according to one of the pre-eminent cardiologists of the 20th century, Dr. Paul Dudley White.
He wasn't talking about ignorance among the general population. He was talking about himself and his peers. They could hardly do anything to treat heart disease, much less prevent it.
That's why they decided to do something about it.
On June 10, 1924, White and five other doctors signed the papers that formally created the American Heart Association. Working together, they hoped, would speed the discovery of lifesaving solutions.

Shortly after World War II, the organization transformed into something bigger and better. Instead of working with and for doctors, the Heart Association reorganized into a public health organization. It began raising funds, then spending that money on research, awareness campaigns and more.
Today, the Heart Association is many things: a leader, a convener, a driving force for the greater good. Yet what's collectively referred to as "the Heart Association" is really the sum of its parts: 32 million volunteers, donors and supporters. That includes generous companies, charitable foundations, fellow health organizations, researchers, doctors, advocates, survivors and more.
Of all the ways to measure progress from 1924 to 2024, the best is probably the death rate from cardiovascular diseases. It's been cut basically in half. That kind of improvement is staggering. We're talking about several million lives saved and improved every year. That's the direct gain. Now widen the circle by including the other people whose lives are enhanced by having those folks around: their children, parents and grandparents; their friends, neighbors and colleagues.
While the Heart Association can't take credit for all the progress, much of what is known about our hearts and brains can be traced to the organization in one way or another. And now, in honor of the 100th birthday, the Heart Association will be celebrating throughout 2024.
It's a time to spotlight the Heart Association's founders and other dynamic figures, such as:
- Eugene Braunwald, who literally wrote the book on heart disease; "Braunwald's Heart Disease" is considered the cardiology textbook.
- Nanette Wenger, a pioneering cardiologist, teacher and leader, who was among the first people to focus on heart disease in women because she understood heart disease wasn't only something that happened to men.
- Edward Cooper, an early advocate for linking stroke and heart disease who became the first Black tenured professor at the nation's oldest medical school, then the Heart Association's first Black president.
It's an opportunity to appreciate the $5.7 billion-plus the Heart Association has invested in cardiovascular research, the most of any entity outside the federal government.
Those investments began in 1948. Progress came quickly. Of course it did. After all, the landscape was like an unplowed field and the soil was getting turned over by scientists who'd been trained by the first generation of Heart Association scientists.
Consider this list of Heart Association-supported breakthroughs from the 1950s and '60s alone:
- The first drugs to lower blood pressure, a landmark study that showed high blood pressure can decrease life expectancy, and the first cholesterol-lowering drug.
- The first successful artificial heart valve replacement and pioneering advancements in microsurgery. These advances led to today's minimally invasive procedures that end a heart attack by inserting stents to clear a blocked coronary artery and a similar procedure that ends a stroke by plucking a blood clot from inside the brain's artery.
- The first external defibrillator and then the first portable external defibrillator, leading to CPR being embraced as a way for anyone to save a life – and eventually, widespread teaching of the technique.
- The first successful battery-operated, wearable pacemaker, leading to these devices routinely being implanted to keep hearts beating at a normal rate and rhythm.
- The first links between fat we eat and blood cholesterol, spurring the Heart Association's foray into dietary guidelines that urged Americans to eat a healthier diet. (In 1973, the Heart Association published its first cookbook. It's still in print, with more than 3 million copies sold.)
- The first scientific statement on smoking and heart disease, a precursor to the landmark report by the surgeon general on smoking and health.
This year also is a great time to explain the depth and breadth of how the Heart Association is working to improve and extend your life.
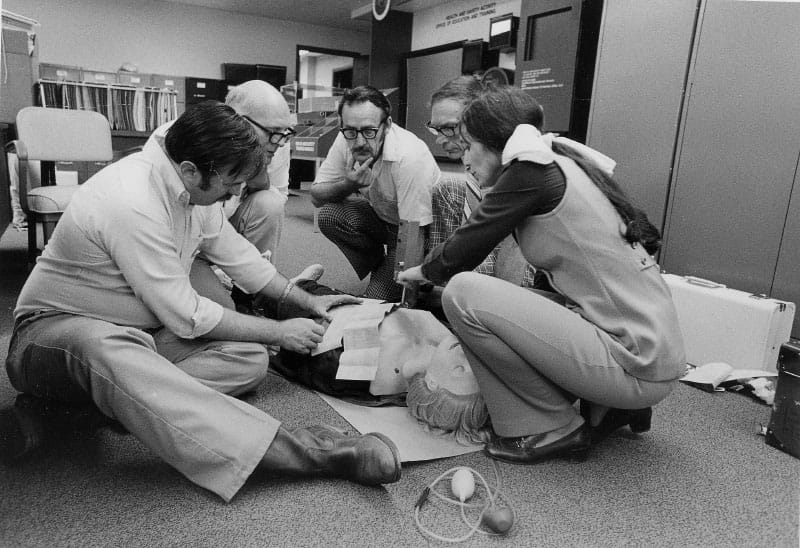
Sometimes the impact is obvious, like CPR classes.
Sometimes it's subtle, like working to ensure you have a safe place to walk.
And sometimes it's profound, like protecting the federal law requiring access to health care for all Americans.
Actually, make that all Americans, a typographic flourish often used to emphasize the organization's commitment to everyone, everywhere getting the opportunity to enjoy a longer, healthier life.
The organization has been working toward the concept of health equity since at least 1969, when the Heart Association created a task force to study why some diseases disproportionately affected certain groups – such as high blood pressure among Black people.
This led to new programs and priorities for the organization, and it set a precedent that continues to be upheld. The Heart Association was addressing "social determinants of health" long before the COVID-19 pandemic exposed those disparities. Seeing that, the organization doubled down on attacking those barriers.
There's another way of looking at the Heart Association's aim of helping all Americans.
It also means the organization cares about you. About improving and extending your life.

The best way to dive into that is by going back to the things mentioned at the beginning of this story: diet, exercise, sleep, not smoking, and controlling weight, cholesterol, blood pressure and blood sugar.
Heart Association-funded research showed those are the key factors to preventing heart disease and stroke. Master those and your chances of a longer, healthier life go way up. That's why they're dubbed "Life's Essential 8."
The organization spreads that information in various ways to various audiences, both in the public and among science and medicine professionals. The outreach to health care audiences is all about making sure newfound scientific findings make the leap from published papers to hospitals and clinics.
The Heart Association – alone, or in partnership with other organizations – is heavily involved in creating treatment and prevention "guidelines" involving cardiovascular care. Quick example: The typical blood pressure target of 120/80.
The Heart Association offers all sorts of programs to help hospitals and clinics follow those guidelines. The organization also certifies care centers best equipped to treat heart attacks and strokes.

First responders know to take patients to those certified facilities whenever possible because it's built into the chain of events that starts with a 911 call. Also built in: Paramedics sharing information with the hospital while they're on the way.
That communication speeds up the "door-to-needle time," which is what it sounds like: logging how long it takes from a patient arriving at the hospital until they get certain potentially lifesaving medicines or procedures. The urgency is for several reasons. The sooner they're delivered, the more effective they are ("time lost is brain lost," is a common refrain of stroke care); also, guidelines are clear that some of those medicines can only be given within a certain time frame from the onset of symptoms.
Getting patients the care they need, when they need it, is a complex puzzle. Sometimes it requires shaping public policy. The Heart Association does that at every level, from your neighborhood to the federal government.
Suffice to say, the organization's impact is all around you.
Now, at the dawn of the Heart Association's second century, leaders are looking forward, focused on advancing health and hope for everyone, everywhere.
As American Heart Association CEO Nancy Brown likes to say, "Our future is about improving yours."
How?
With more cutting-edge research. With new technologies. With approaches so innovative they don't yet exist.
Heart Association volunteer president Dr. Joseph Wu is among those creating the future. He runs the Stanford Cardiovascular Institute, and one of his projects is studying the effects of zero gravity on the heart in preparation for the day when space travel becomes routine.
It's with that spirit, during his speech at Scientific Sessions, that Wu mused about what may be in store.
"Who knows? 100 years from now, this great organization may be celebrating its 200th anniversary on the planet Mars."






