Heart failure at 25 cost her three limbs. Now she’s rebuilding her life with strength and hope.
By Deborah Lynn Blumberg, American Heart Association News

Working from her home in Phoenix, 25-year-old Alyssa Reader felt unusually anxious.
She put her marketing project aside and texted her mom, Natalie Reader, who lived a few minutes away.
“I feel weird. Not sick, just off,” Alyssa wrote.
“Come over,” Natalie responded.
So Alyssa scooped up her dachshund mix, Winston, and drove to her parents’ house. She collapsed onto the couch and rested for a few hours. She felt well enough to attend a friend’s going-away party. The next morning, she felt worse.
Natalie took Alyssa to urgent care. Alyssa’s heart rate was so high – nearly 140 beats per minute – that the doctor sent her to the hospital. Further testing found … nothing.
“You can go home,” the emergency room doctor said. “If you feel worse tomorrow, come back.”
The next morning, while showering, Alyssa had trouble standing. Natalie took her back to the ER. This time, tests showed she had very high levels of troponin, proteins that release when the heart muscle has been damaged.
Doctors said Alyssa had pericarditis, the swelling and irritation of the thin, saclike tissue around the heart. They couldn’t explain what caused it.
Not long after Alyssa was admitted, a nurse came by to take her blood pressure. The machine couldn’t get a reading.
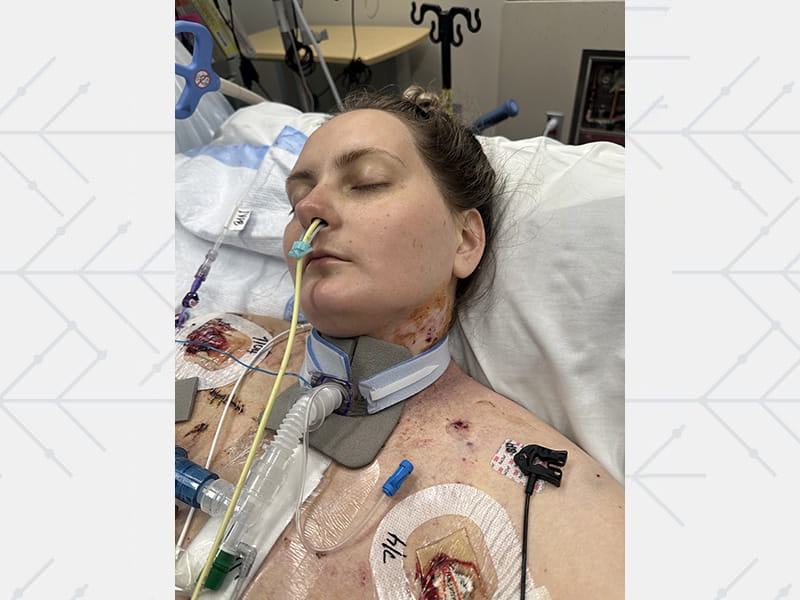
“It must be broken,” the nurse said.
A second nurse arrived with a new machine. It couldn’t read Alyssa’s blood pressure either. The nurse stepped out.
Within minutes, more than a dozen doctors and nurses swarmed Alyssa’s room.
The problem wasn’t the technology. It was Alyssa.
The left side of her heart was failing.
Doctors connected her to a machine that provides a form of temporary life support that oxygenates blood outside the body and circulates it back to the patient, a process called extracorporeal membrane oxygenation, or ECMO. They also implanted a temporary heart pump. The combination was supposed to allow her heart to heal.
It didn’t work. Even worse, the right side of Alyssa’s heart began failing, too.
She went to yet another hospital, where doctors opened her chest and placed ECMO directly into her heart.
“Alyssa has a 10% chance of survival,” a surgeon told Alyssa’s loved ones, a group that now included both her parents (her dad, Shawn, flew in from Virginia, where he’d been working), her 21-year-old sister Karli, childhood friends and co-workers.
Family and friends said their goodbyes to Alyssa.
The new, more direct version of ECMO worked. A week later, her surgeon lowered the ECMO to test her heart function. It was beating strong. He removed the ECMO tubes.
Then came a startling discovery.

Blood wasn’t flowing through Alyssa’s legs or right arm. To live, she needed her legs and right arm amputated.
“She’s 25, I don’t know if she wants to live like that,” Natalie responded, through tears.
She talked it over with Shawn and Karli. They decided Alyssa would want the surgery.
Hours before the operation, Natalie sat by Alyssa’s bedside. Alyssa was in and out of consciousness. “Do you want everything possible done to save your life?” Natalie asked.
Alyssa squeaked out, “Yes.”
The surgery went according to plan.
After a month in the intensive care unit, Alyssa started physical rehabilitation. She received prosthetics. In December 2024 – six months after she was first rushed to the ER – Alyssa moved into an accessible room in her parents’ home.
At first, Alyssa wasn’t in the mood to leave the house. She worried people would stare at her. Her only change of scenery was car rides with family and friends. On Christmas Eve day, she built up the courage to visit a home goods store. Hardly anyone looked at her as she browsed the aisles, which helped her feel better.

In February 2025, Alyssa took her first steps with prosthetics. As a triple amputee in heart failure, her progress has been slow. She gets fatigued easily as she builds her muscle strength up from zero while re-learning balance and endurance.
Alyssa continues working with a physical therapist three times a week, walking and now incorporating balance and strength training into sessions.
“Alyssa has a lot of grace,” Natalie said. “Something like this can make you super bitter against the world. But Alyssa doesn’t sit in a corner kicking and screaming and saying ‘Why me?’ It’s, ‘These are the cards I was dealt, and we move on.’”
Alyssa dealt with heart problems during her post-surgery ICU stint and again after returning home. She even had to be hospitalized again.
Now, a small device recently implanted in her pulmonary artery sends pressure readings to her care team each night. The remote monitoring allows health professionals to spot changes early, often before her symptoms worsen, and adjust her medications right away, helping to keep her out of the hospital.
Perhaps the best way to appreciate the turnaround in her condition centers on her ejection fraction, which is essentially how efficiently the heart muscle is squeezing. Normal range for adults is 55% to 70%. At her worst, Alyssa’s EF was 3%; it’s recently been as high as 49%.

Now 27, Alyssa’s goal is to live independently and to drive.
Seeing other amputees on social media living on their own and enjoying hobbies like hiking makes her think she can, too.
“Everybody rooting for me has helped me to be in a positive space,” Alyssa said. “As traumatic as everything was, I’m so lucky and blessed to be alive so I can keep creating memories with my family and friends. I wouldn’t have survived this without them. I truly feel like I made it for a reason.”
Stories From the Heart chronicles the inspiring journeys of heart disease and stroke survivors, caregivers and advocates.
The heart is a muscle and when it doesn’t work properly, it’s not pumping enough oxygen-rich blood to the rest of the body. This is what’s known as “heart failure.” Learn about the condition, your risks, treatment options and more.





